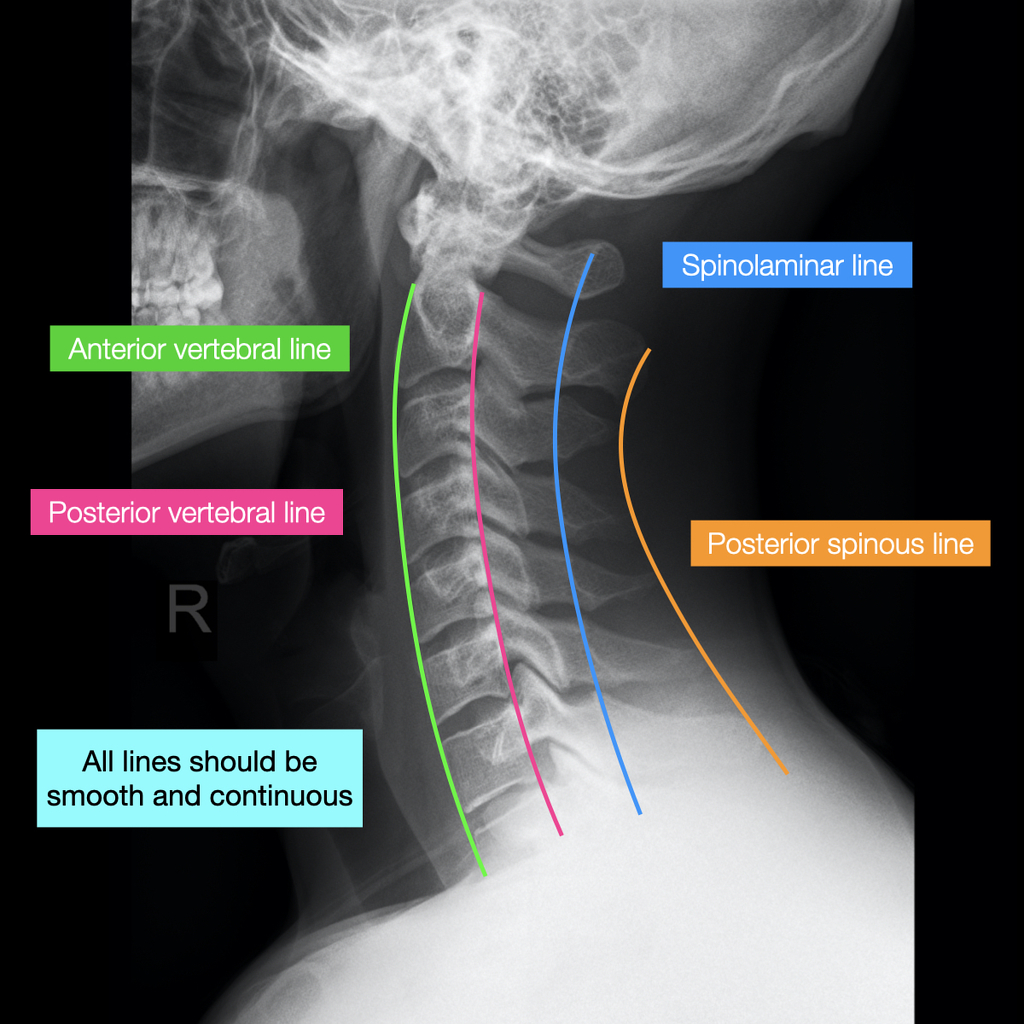
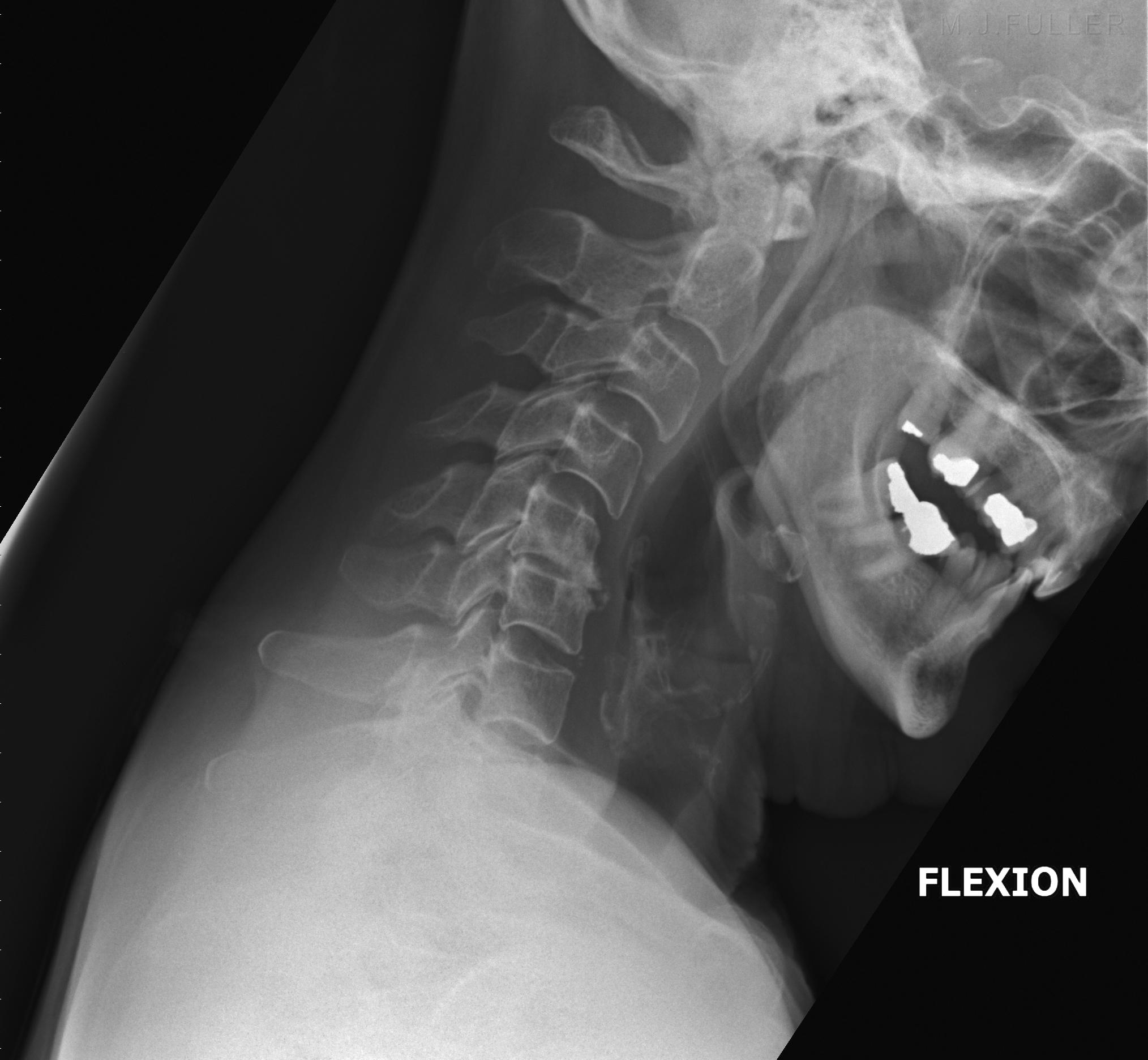
Sclerosis of bony margins and the presence of widespread degenerative change can assist in the differentiation of acute from chronic processes. Calcification of the anterior longitudinal ligament.A variety of radiographic features indicate pre-existing degenerative processes, including: Plain film radiography may also reveal the degenerative changes common to older people. Soft-tissue swelling may be evident, and this too requires further evaluation by additional views or alternate modalities to rule out a significant fracture or instability. Radiographs help to rule out fractures or malalignment of the cervical spine. If the lordosis reversal is accompanied by swelling along the anterior longitudinal ligament, significant regional trauma may be present. Young people in particular can often reverse the lordotic curve with the simple instructions to sit tall and tuck in their chin. Radiographs may show a non-specific loss of normal lordosis or straightening ( Figure 1) but alone do not indicate a specific diagnosis of whiplash. However, if there is any suspicion of a fracture or instability, clinical judgment is still the overriding principle and radiography must be carried out while ensuring immobilization of the cervical spine. Though it must be emphasized that these features have yet to be validated, a patient involved in a simple rear-end motor vehicle collision who later presents with the complaint of neck pain may not require radiographic evaluation. In addition, radiographic evaluation is recommended for any patient where active neck rotation cannot be completed by the patient in the defined manner. Plain film imaging is also recommended in the setting where examination of the neck is unreliable, such as with distracting painful injuries elsewhere, altered level of consciousness, or evidence of facial or external head injury. Radiography is recommended when high-risk factors are present, such as age greater than 65 years, a defined dangerous mechanism (see the Table), or any report of a sensory abnormality or focal neurologic deficit in the extremities. Then, when an evaluation occurs in a broad range of settings given the identified low-risk factors, it is postulated that the ability to rotate the neck may reliably predict all individuals who do not require radiography. The next step in the process of validation will be to ensure that these low-risk criteria can also be applied in the settings of community hospitals and primary clinics. Investigators in the CCC study are currently completing a multicentre investigation in Canadian urban teaching hospitals whereby a set of low-risk factors can predict the selection of patients who can then be allowed a supervised assessment of range of motion. The CCC (Canadian C-Spine) study under the direction of Ian Stiell at the University of Ottawa is in the advanced stages of validation in Canada, with a current enrollment of 14 000 patients. The NEXUS study, a decision rule cervical spine radiograph study, has received wide interest in the United States. Initiatives are under way in Canada and the United States to help identify the groups of patients with blunt trauma (whiplash associated disorders, WAD I and less commonly WAD II see the Table in the article "Incidence of whiplash-associated disorder" for a definition) where the history and physical examination can clearly exclude significant pathology.ĭecision rules regarding the need for radiographs are being validated that will allow selective ordering of imaging studies. Simply stated, radiography is indicated if the possibility of a fracture exists. It is recognized that patients sustaining a cervical injury (whiplash) from a rear-end motor vehicle collision may be seen in a variety of settings including emergency departments, family doctors’ offices, and clinics. Some authorities still recommend the routine inclusion of plain film radiography for any case where trauma to the neck occurs and the clinical finding of midline posterior neck tenderness is present.
Avoiding radiographs for those patients where the results are predicted to be normal translates to significant savings to our medical system and a reduction in the exposure of patients to ionizing radiation. An estimated 200 000 radiographs of the cervical spine are carried out annually in Canada on patients who have been injured through blunt or secondary trauma to the neck. The indiscriminate use of radiographs has been primarily driven by the ever-present concern of cervical spine stability.
